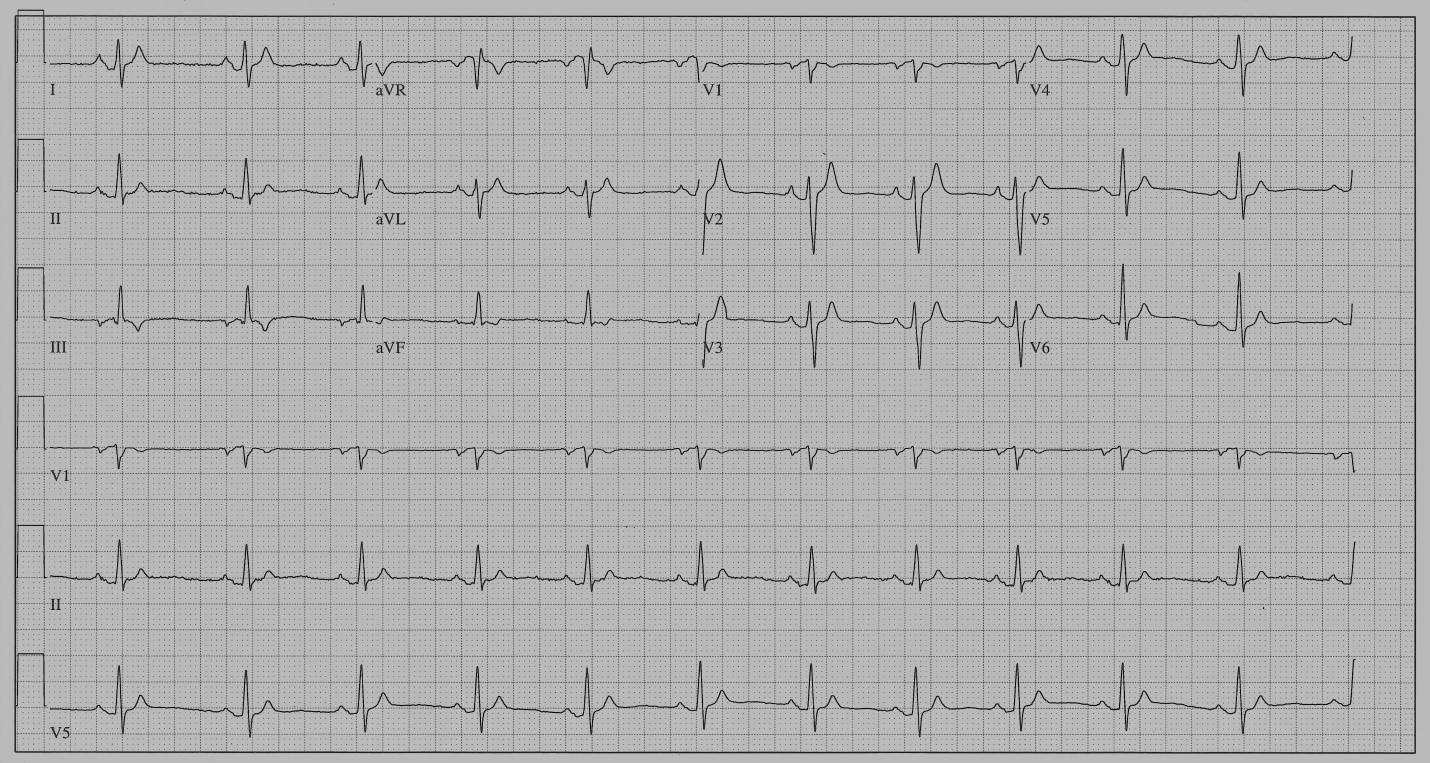
Regarding the second part of the maxim, “you recognize what you know,” there are several issues regarding the QT-interval that are important to be aware of when making the diagnosis of SQTS. As shown by exercise testing of patients with SQTS, the QT interval alters very little with changes in heart rate. A recent exercise test study from five European Centers of 21 patients with SQTS (QT: 276 +/- 27 ms) and 20 healthy subjects (QT: 364 +/- 25 ms) found a QT-HR slope in SQTS patients of -0.53+/- 0.15 ms compared to -1.29 +/- 0.30 ms in healthy subjects.46 Because of a difference between the two groups, not only in terms of SQTS, but also short QT intervals, it is difficult to tell whether the variations in HR-QT slopes are due to the difference in QT interval duration, or SQTS. It may therefore be too soon to fully accept the authors suggestion, that, “in subjects with QTc intervals between 340 and 360 ms, the presence of a QT/HR relationship slope under -0.9 ms.beat/min could help distinguishing affected subjects from healthy individuals.” Until a comparison of patients with SQTS and healthy individuals with similar QT-intervals have been studied we cannot be certain whether the HR-QT slope can be used as an aid in diagnosing SQTS. An important consequence of the diminished effect of heart rate on the QT-interval in patients with a short QT interval is that correction calculations based on Bazett’s formula will overcorrect short QT intervals to a much higher degree than in people with normal QT intervals. At slow HR’s this may lead to over-diagnosing SQTS, and at fast HR’s to under-diagnosing SQTS.
Despite these well-documented shortcomings in using QTc especially in patients with SQTS, QTc is commonly used in recommendations on SQTS diagnosis. In order to avoid extreme overcorrections by this method it is, however, recommendable to obtain an ECG at a heart rate as close to 60 bpm as possible (repeat ECG, Holter) and limit the use of Bazett’s correction formula in diagnosing SQTS to heart rates between 50 and 70 bpm. It is also unrealistic to expect that a single QTc value will distinguish all cases of SQTS from healthy individuals. Since the HRS/EHRA/APHRS Expert Consensus Statement on the Diagnosis and Management of Patients with SQTS from 2013,47 there has been two major studies with new information about SQTS suggesting that an update in criteria for diagnosing SQTS would be appropriate. Prior to 2013 only 5 of 70 SQTS patients with information of individual QTc’s had a QTc > 330 ms . Since then two multicenter trials including 126 patients,23,38 have used QTc ≤ 340 ms as stand-alone criterion for making the diagnosis of SQTS. In one of these studies where individual QTc’s were given,38 21 out of 73 patients, of whom 84% were male, had QTc > 330 ms while all of them had a QTc ≤ 360 ms. Based upon these data it might be appropriate to use QTc ≤ 340 ms as stand-alone criterion for SQTS. In addition, based upon recent data from the largest SQTS family published so far, where four (all males) out of twenty-three mutation-positive patients (17%) had a QTc ≥ 360 ms, the upper limit for QTc should probably be 370 ms instead of 360 ms when SQTS is diagnosed in the presence of one or more of the following: a pathogenic mutation, family history of SQTS, family history of SCD at age ≤ 40, survival of a VT/VF episode in the absence of heart disease, atrial fibrillation at a young age and syncopal episode that strongly suggests a cardiac arrhythmia. In comparison to the 2013 guidelines atrial fibrillation at a young age has been added based upon the discovery of KCNQ1-V141 mutation positive children with atrial fibrillation, and the addition of syncopal episodes is based upon three multicenter studies21,23,38 which includes the majority of patient data published to date. In the first study syncope was not defined, in the second study syncope had to be of arrhythmic origin and in the third study syncope was defined as a transient loss of consciousness in the absence of alternative explanations (e.g., labyrinthitis, orthostatic hypotension, or clear, vagally mediated events).